 This is a parent’s worst nightmare and it is often compounded by the next words from the doctor’s mouth. “He will have cerebral palsy. This means he probably will not walk, talk or attend a normal school. We will have to wait and see how bad it will be.” If you were told this in the difficult early days, it is almost impossible to get rid of it. It lurks about at the back of your consciousness and even years later, many parents are still waiting for the proverbial shoe to drop. The big question persists. How bad will it be?
This is a parent’s worst nightmare and it is often compounded by the next words from the doctor’s mouth. “He will have cerebral palsy. This means he probably will not walk, talk or attend a normal school. We will have to wait and see how bad it will be.” If you were told this in the difficult early days, it is almost impossible to get rid of it. It lurks about at the back of your consciousness and even years later, many parents are still waiting for the proverbial shoe to drop. The big question persists. How bad will it be?
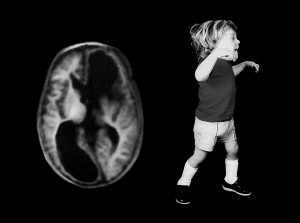
So, take a big breath and relax. This is an outdated, incorrect statement. The boy with the extensive brain damage shown in the image, did develop cerebral palsy, but it was mild. GMFCS I. There have been big changes in the cerebral palsy world over the past 20 years or so. The first change is the growing awareness of neuroplasticity – the ability of the brain to regrow, repair, reorganize and reallocate resources to create function. read…Real or False Hope after Early Brain Damage?
Once the regenerative ability of the brain is recognized, then new approaches and treatments are possible. We now know that neuroplasticity is stimulated by novel, challenging tasks with consequences. Great news…but it comes with a catch. It demands a major change in the mindset of doctors, therapists and educators in the CP world. It really demands a shakeup of their worldview. I hope that parents everywhere are encouraged to talk about my book and even consider it as a great holiday present for their healthcare team. The Boy Who Could Run But Not Walk: Understanding Neuroplasticity in the Child’s Brain , is the story of the long road to my own mindset change from thinking that the only option was to prevent baby brain injury to the new mindset of challenging the negative prognosis with innovative approaches and treatments. Dr Dweck’s book, Mindset, is another of the must read books in my parent survival kit.
I have a question for you. Were you given a similar dismal prognosis? If yes, I would love to hear your story on my Facebook group.
I am halfway through your book. You hade me cheering in the first few pages. Our daughter is 3, diagnosed at 2 with mild CP. when I asked the doctor whatnher prognosis was, she said “she will probably always be a little clumsy and she probably won’t want to join any team sports…she wouldn’t want to let her teammates down.”
We switched doctors.
We credit therapy since age six months for her progress thus far but have seen continually the idea that “she will always be this way.”
We couldn’t understand that given adult stroke victims who recover so well. Finally, you have answered that question. Thank you!
We immediately sought and found a physical therapist who understands gait training. I gave her a copy of your book. Turns out, she once attended one if your courses on EStim! Thanks so much for your book and sharing your research.
We are telling every healthcare member about your book.
Thank you for your uplifting message.I am pleased things are going well.Norman Doidge’s first book, the Brain That Changes Itself, changed the world of adult stroke rehabilitation as the families and general public learned more about adult neuroplasticity. My hope is that my book will work a similar miracle for CP rehabilitation.Thank you for spreading the word.
We were given graciously the news that in time the diagnosis of cerebral palsy will most likely be the case. Our docs have always waited for us to ask questions rather than telling us how its going to be. What’s been hard is explaining things like tone and how the CP manifests in an infant (even in the eye muscles) to my mother who is always so proud of my daughters physical “strength”.
You might share your copy of my book with your mother…it is helpful for grandparents to learn more about the condition.
Best wishes
Our son is 8 years old. He had breathing problems after birth and was in NICU for 6 weeks with many apneas. When he was 3 days old, a doctor told us that he would never be able to feed orally – that was so discouraging to hear! He was wrong! Soon after birth he was diagnosed with Muenke syndrome (with cranio-synostosis, and he’s never had surgery for that since it would have purely been for cosmetic reason), severe hypotonia, and a few other things. Within the last 1.5 years, he was diagnosed with severe growth hormone deficiency, Autism Spectrum disorder, intellectual disability and Prader-Willi Syndrome (which impacts the brain). 14 months ago our family went to IAHP (www.iahp.org) re: neuroplasticity and to have them assess our son and design a program for us to do with him, and since then we’ve had him home full-time to work on as much of that program with him as we can. He had taken JK and SK (1 year behind his age) prior to that, in a private school, with a 1-on-1 EA/PSW. We’re currently planning to continue our neuroplasticity therapy with him for at least another 1-2 years (based on IAHP, although we may research/apply other neuroplasticity things for him as well). When we started neuroplasticity therapy, we stopped SLP, but we’ve done some PT. We’ve never done ABA (behaviour therapy) with him and don’t currently plan to, since we want to heal his brain (the root cause) rather than try to just treat symptoms. When our son was much younger, we didn’t know if he would ever be able to walk. Our son wears SMO’s and shoes most of the time (including in our home) and he can run on flat surfaces with his SMO’s and shoes and he can walk up and down stairs while holding a railing! Our son loves to read! And he loves music and sings incredibly well!
Good to read your story.Now that he is up and moving, it is worth seeing a good therapist to see if any of his aids need upgrading. I would also ask about compressive garments may help with the low tone of his P-W diagnosis. It is always hard when the child has multiple diagnoses.
Where do we start? I have a grandson with CP and we live in Iowa.
I would read my book and share it with your healthcare team. You could also join my Facebook Group and read the input from other parents and grandparents.
https://www.facebook.com/groups/Karenpape/
Hi Karen,
I recently read your book, my son had moderate to severe HIE at birth and all we were told was wait and see. He is now 14 months and has not met any of his motor skills related milestones. He is doing ok congnitively but behind on that as well. After reading your book I am desparate to find alternatives, as time is of the essence and give he understands things I have hope that he can recover. He is in all kinds of early intervention therapy but unfortunately not seeing much progress. I would love to have some sort of plan for this year given how this year is so critical for him, who else do I go to, what other specialists can I talk to? I feel like he needs more than the EI therapy he is currently getting, would appreciate direction and advice
Dear Anamika,
Most Early Intervention programs are treating a child for “Developmental Delay”. I think the advice you are being given is helpful for his cognitive development, but you should ask your physicians for a diagnosis of his motor delays, mostly like a form a form cerebral palsy, and get some lesion specific therapy from a physical therapist. Waiting for a firm diagnosis makes no sense to me. If they say it is too early to be sure, get a label of “at risk of cerebral palsy”. The important part is getting the PT who knows what to do working with you.
Hope this helps,
Karen Pape
Dear Karen
Thank you for your work and your inspiring vision to help children and families facing brain injury. I was so sorry to hear that you haven’t been well recently. I wish you good health. I had a very traumatic indentical twin pregnancy and twin to twin transfusion syndrome set in at 20 weeks. Following placental ablation surgery we lost one twin. I had to carry both babies to the end and I suffered proms and a haemorrhage at week 31 & emergency c section delivery. Our surviving son did well in NICU only intubated over night as he pulled it out & then oxygen therapy, caffeine, phototherapy & time to establish feeding once the feding tube was removed. He stayed a total of 6 weeks and finally came home with us. He had brain ultrasounds on the unit and nobody even mentioned cerebral palsy or any kind if brain injury so we believed we were in the clear. At ten months he was still not sitting up. Very smiley and responsive but Just lying on his back & not even rolling. We took him back to hospital and a MRI head confirmed mild bilateral PVL and thinning of the corpus calosom. We were devastated. Such a shock. Consultant gave us the results over the phone and said i cannot gaurantee he will ever walk or talk. We were then referred to a paediatrician at a neuro development center for children who met with us for a hour and told us to be positive, see how he goes come back in 6 months. We read your amazing book and began physio, swimming, hydrotherapy and just recently been assessed for conductive education. We still haven’t seen a neurologist or anyone to actually talk through the MRI in detail and we still await lots of referrals ie speech and language and Occupational therapy for some possible equipment like a bath seat etc. He is strong and moves all his limbs well but only when lying down. He curls his toes and has low tone. The wait for services on national health service for children is painful and it seems like 50 percent of paediatric referrals either don’t get made or they get lost. I am constantly pushing. Our son has responded to Physio slowly and can now sit unaided for 6 seconds. He still gets around in his own way scooting on his back. I’m worried that these pathways are just getting stronger and stronger as time passes. He is very affectionate, loves looking at books (on his back or in supported sitting) he loves music and smiles when we sit close to the sea. He points at the waves and smiles. He is now 15 months old. Any advice would be so gratefully received. Your book has been the only ray of light during this painful time. Thanks for your amazing work. We live in Eastbourne in England, UK. My sons name is Jude. We adore him. Thank you Karen, sorry for a long post. Best wishes for your full recovery
Thank you for you post Sadie. I am sad to hear that the NHS is still so slow. I did a post-doc in London in the late 1970s and it was as you describe then! So, it just makes my point that change will only come when parents unite. Look at this blog and discuss with your physiotherapist.http://www.karenpapemd.com/good-enough-is-not-good-enough-any-more-function-follows-form-in-cerebral-palsy/ Hope this helps, Karen
I would keep pushing for a diagnosis. It is good that he is responding to the phsio. Ask if some trunk support would be of help.http://www.karenpapemd.com/good-enough-is-not-good-enough-any-more-function-follows-form-in-cerebral-palsy/
I forgot to say in
My previous post the conductive educator put our son on a big yoga ball holding him by the hips and said she could feel a little bit of spacticity in his ankles, legs, hips and a tiny bit in the shoulders. She said he was a typical presentation of CP. what type of CP does this sound like? Are you able to comment/advise us? Best wishes xx
If I made a guess it would be preterm pattern diplegia, but you should push for an appointment with a neurologist. Diplegia is the most common type of CP in the ex-premature and the outlook for it is good. http://www.karenpapemd.com/cerebral-palsy-diplegia-gmfcs-i-to-iii/ and http://www.karenpapemd.com/title-will-my-child-walk-are-we-doing-the-right-therapy/
Hard to tell without an examination. I would ask your md’s.
Hi both, sorry to hijack your conversation but I think I have something to add. My daughter has CP GMFCSIV and was written off by NHS at 2, saying this is the best she’s going to be. We went to a school for conductive education. In the 12 months she’s been there she’s changed beyond recognition. She speaks like a 3 year old from nothing, she weight bears from nothing. She sits with a little support from nothing. The conductors are obsessed with meuroplasticity and repeating a good movement to get those cells to grow round that impulse. It works. Don’t give up. Sent with love and light.